Seeking better payer-provider relations: An interview with Dan Unger, Chief Product Officer, Anomaly.
- Eric Fontana

- 3 days ago
- 11 min read
For those in healthcare, and revenue cycle especially, your newsfeeds undoubtedly provide a consistent stream of stories illustrating abundant payer-provider friction. Few would argue the most visible of these tensions has been around health system and clinician reimbursement for services, which has catalyzed a rapid investment into AI-tech on both sides, often described by one of many possible wartime analogies, although yet to have reached the point that either party appears ready for armistice. Amidst the “sticks and stones” chaos are some key players aiming to find some sane middle ground. Dan Unger is the Chief Product Officer of Anomaly. We caught up recently to chat about how deeper analytics could help rationalize reimbursement with contracts more promptly and potentially bring each party to the table to spark meaningful collaboration. We also touch on what we’re more and less hopeful about as we peer into the future of how the current tension progresses.
Bridging a gap between payers and providers to help eliminate unnecessary friction and costs
Eric: G’Day Dan! Can you kick us off with some high-level background on Anomaly, your role, and what you are trying to improve?
Dan: Anomaly was founded about five years ago as a Redesign Health-backed company, and I joined as Chief Product Officer roughly 2 years ago. The initial remit – before my time - was to use machine learning and AI to prevent fraud, waste, and abuse on the payer side. Over a few years, the team realized the core data model and machine learning algorithms for understanding claims data would be very useful for providers and that’s our focus today. We pivoted to address the $300 billion in administrative waste in healthcare caused by middlemen fighting in a complicated payment system. Our goal is to be a trusted broker that provides a shared source of truth for payment rules and medical policies. We hope to meaningfully eliminate unnecessary admin costs, ideally taking it down by getting 90% of it right.
But we know the world isn't quite ready for that yet, so we started by helping providers reverse engineer what payers are doing. This helps them improve internal processes and level the playing field in negotiations by bringing "the receipts" to conversations. Eventually, we hope to bridge the gap so everyone realizes it’s a zero-sum game and can work together peacefully.
The denials and visibility challenge: Inconsistency and lack of transparency makes it difficult for providers to stay on top of everything
Eric: Do you see one of the fundamental challenges for health systems right now simply being visibility into payer behavior?
Dan: Absolutely. We see dozens of revenue cycle and technology vendors, yet denial rates, takebacks, and downgrades are getting worse. It’s not because the vendors or health system experts are bad at their jobs; it’s because you cannot fix what you do not understand. Our hypothesis is that shedding light on these behaviors is key. Sometimes the issue isn't even behaviors, but rather the "source of truth" within crazy payment models and medical policies. Shedding light on what is happening and why allows you to decide if it should be happening in the first place.
Eric: Since you have been tackling revenue cycle challenges, is there anything that has surprised you about the nature of the denials problem?
Dan: A few things have been surprising. First are the inconsistency and lack of transparency in what a payer tells a provider, such as using vague or inappropriate reason codes. This makes it hard for providers to understand what to do about a given denial, or how to build workflows around them. Second, we see many denials that are actually valid and preventable coding and billing edits. The real problem is that inconsistency across payers makes it impossible for providers to edit every claim for every known policy; they would never get a bill out the door.
Third, denials are just one part of the equation, as payers are becoming more creative with downgrades, like automated ED downgrades or downgrades on, say, $90 office visits. They are also doing bulk retractions and takebacks, sometimes hiring vendors to perform audits that result in $8 million adjustments out of nowhere. Payers are also shifting patient responsibility onto providers. When you add it up, it’s wild that health systems stay afloat given everything thrown at them just to get paid.
Payers targeting exposed areas in the traditional provider playbook
Eric: Quite often when you and I speak, you’re elbows deep in data: 835s, 837s, CARC, RARCS, reason codes and more. What's some insight from your analytics that you think many in the industry might not be fully aware of?
Dan: The data is pretty clear, we are seeing insurers start to attack higher volume, lower dollar services. For example, some payers hire vendors with opaque rules for labs that no health system can afford to fix because it’s a $20 claim. Health systems are often very good at the inpatient side because they can afford the technology and documentation experts there. However, they cannot afford the same resources for a $1,200 outpatient claim or a $50 lab claim. Payers are going to these "fringes" because they are machine-scale problems that health systems can't keep up with. People feel they are getting hammered, but it’s hard to see because it’s not $1 million NICU claim, but 14,000 denied labs.
Eric: Is it fair to characterize these types of behaviors as a direct attack on the traditional provider playbook, as payers seemingly aim to hit known weak points in a health system's defense?
Dan: For sure. Carriers claim providers are "upcoding," but providers have just gotten really good at coding appropriately after ICD-10. If it were truly fraudulent upcoding, the payers would do something about it. Instead, they go after areas where providers are weakest because they cannot afford to throw people at low-dollar volume.

Providers “getting their house in order” as payers ramp up AI tactics
Eric: It feels like an unanticipated consequence of provider AI use is that dollars previously assumed to be left on the table, are now being accurately captured, and payers are pivoting to more active approaches for recoupment…
Dan: Agreed. They are doing it through low-dollar areas and information requests. Some payers hold up 15 to 20 cents of every dollar by asking for medical records or itemized bills. This delays payment, causes things to fall through the cracks, and allows them to pay less by crossing off items or claiming they are bundled. Providers have little leverage right now because nothing in the contract prevents this behavior.
Eric: How would you characterize the importance for health systems to root-cause their denials today - to identify key areas for prevention - to see if it is a "me issue" or a "payer issue"?
Dan: Oh, extremely important. Especially when you think about where the market has moved and what it means for problem resolution with payers. You don't want to be the "boy who cried wolf" at the negotiation table by bringing up things that are not the payer's fault. So, step one is identifying what is in your control and what is valid. Once health systems have dealt with these, you’re left with the truly important payer issues to focus on. Where we’ve seen success, is in situation where we’ve presented a small number of deeply validated issues rather than a much larger number of one-off complaints. We separate valid payment integrity rules that the provider needs to fix internally from the areas where the payer is hammering them unfairly. We try to sift reality to see if there are collaborative issues, where data sharing can help, like tricky eligibility or coordination of benefits issues. In short, cleaning up your own house, then make sure whatever is a payer issue is airtight before presenting it to the payer.
Eric: So, if you’re a health system that has “gotten your shop in order” so to speak, what approaches are subsequently available for changing the payer-provider dynamic through detailed analytics?
Dan: One way we’ve worked with health systems is by bridging the gap between the revenue cycle data seen on the ground and what managed care needs for meaningful conversations. The gap in basic reporting was much bigger than I thought. There is a translation problem where managed care has an 80+ page contract and dozens of spreadsheets, while the revenue cycle has 32 different payer IDs in Epic. When a payer asks specifically where a problem is happening, and that’s asking for the plan or adjudication system level - the provider often won’t know the answer. If you can't answer those next-level questions, the conversation is dead. Bringing basic analytics to tease out lines of business and remark codes moves the needle.
Eric: So, the key is being buttoned up on information and presumably anticipating the next questions…
Dan: Exactly. You need data to show if a problem is national or specific to them, and you need examples ready to go. We use human validation to review cases against policies and contracts so the issues we bring are rock solid. If you want to move the payer from curious to action, you need a compelling case and to put the ball in their court.
Eric: Have you seen payer receptivity when you’ve pointed these issues out with data?
Dan: For sure, we’ve had some encouraging success. When you are right and have the data to prove it, payers often listen because obviously they don't want to do anything illegal and many still want to work collaboratively with providers. And the interesting thing is that more often than not, payers don't even know these things are happening because they are so big and have outsourced processes to multiple payment integrity vendors.
For example, in one case we found a plan with a denial rate for chemo and immunotherapy that was 20 times higher than other payers, holding up $40 million a year. It was taking six months to get paid, even though they eventually paid 90% of the time. We identified the outlier behavior, reviewed charts, and proved it was a payment integrity vendor edit that wasn't valid. The payer told their (payment integrity) vendors to back off and made amends with the health system by fronting them payments while they worked to resolve the issue. In another case, we unwound itemized bill edits that a payer was using to inappropriately claim services were bundled. Once we brought the receipts, they shut off the edits, saving the health system millions. They’re good examples of how presenting the right detail to support the identification of a problem can work.
Eric: Presumably, being buttoned up creates an additional halo benefit where the payer realizes you – the health system - are not an easy target and takes some scrutiny off.
Dan: Yeah, that’s an important part of the equation. We have definitely seen that dynamic play out. Some people try the automated appeals route, but that is just "spray and pray." Appeals are actually a bad process for everyone because they often cover up poor internal processes. If an appeal is overturned, it means the work was valid, but the claim structure or coding was wrong. It’s probably far better to fight in bulk at the executive level with data than to engage in "guerrilla warfare" on every single claim.
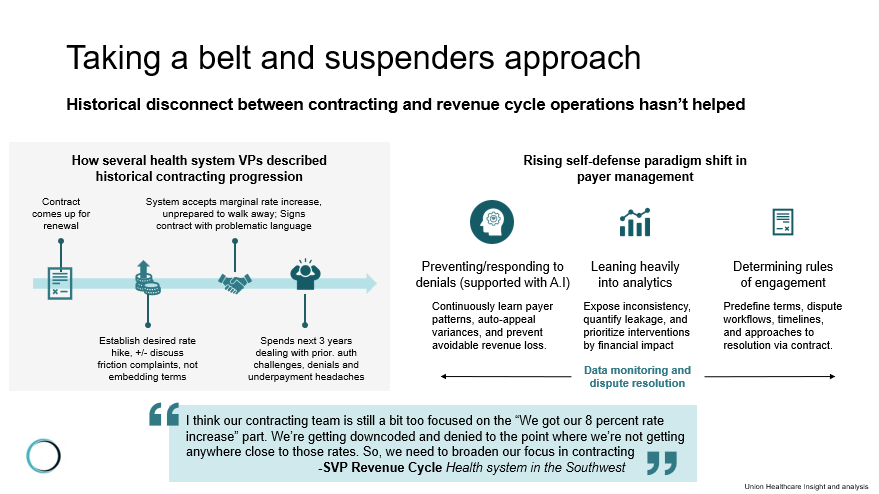
Parting thoughts: Peering into the future of payer-provider relationships, AI, and more.
Eric: Where do you think the industry will be in five years regarding the use of AI in adjudication, audits and takebacks?
Dan: I actually don't think payers are using AI as broadly as they could be just yet, because they don't need to; they’re still primarily using hard-coded rules and edits to not pay claims. Where AI should be used is for frictionless payment, sharing policies and documentation for seamless transactions. In the short term, I'm more worried about payers using the opacity of contracts to "make s*** up" rather than using AI.
For example, one payer we found in our data rolled out a policy to only pay for the highest procedure in an outpatient setting, which is like going to dinner and only being charged for the lobster while the steak and appetizers are "free." These policy changes are way more impactful than AI bots. My hope for five years out is that everyone gets sick of this game and realizes there is a better way. We have the tech to know what occurred and what should be paid without a human touching it. It’s not a tech problem; it’s a lack of trust and an intentional impossibility in the current system.

Eric: Let’s pivot a little. We talk about financial exposure for health systems, but I do suspect there’s risk of over-indexing on denials and underpayments at the expense of the patient collection dynamic as an underappreciated financial exposure? I’m not suggesting health systems go after patients, but more posing why health insurance behaves differently to other categories of insurance when it comes to deductible behavior and who is left holding the bag.
Dan: I think it’s the silent killer. Many people have initial denial rates of 10% and fight them down to 2% in write-offs. However, some payers have 10-15% of the negotiated rate as patient responsibility, and health systems write off 40-50% of those collections. That is a 4-5% yield loss, which is double every other denial category combined.
Providers need to start going after this in contracts, perhaps with triggers that increase rates if patient responsibility exceeds a certain threshold. There are better, co-pay focused models that reduce exposure for providers. Currently, it costs more in write-offs than the entire revenue cycle function itself. It’s an emotional distraction; providers complain about payment integrity rules that represent 1% of dollars, while they are losing 12% to patient responsibility.
Eric: And presumably with more procedures moving to the ambulatory realm, this will only grow in importance as health systems experience “mix-shift” given their historic reliance on procedures, now open to more competition for margins.
Dan: Oh yeah, for sure.
Eric: Let’s wrap up with one last question. What makes you more and less hopeful for the future of payer-provider interactions around reimbursement?
Dan: Let's start with the bearish perspective: The current payment system, the most absurdly complicated and convoluted payment system mankind has ever created, is deeply entrenched in the core systems, processes and legal contracts of a $5 trillion industry. Unwinding that culturally, legally and technically, which is what truly needs to happen to eliminate all this waste, feels nearly impossible on most days. Additionally, the entire healthcare and health insurance payment industry is built around taking advantage of this complexity. It’s an industry that employs millions of Americans and has created dozens of multi-billion-dollar companies. These entrenched interests will fight extremely hard to keep things the way they are.
On the hopeful side: The current national scrutiny and momentum around this problem is something I have never seen in my career. Between government policy trying to tackle the issue, grassroots movements making real headway, national news stories digging deep into the issues, lawsuits on all sides of the aisle, people like Mark Cuban stepping in and screaming from the mountain tops...it really seems like people understand the problem and are willing to fight for change.
Additionally, the rapid improvement in technology and AI is a double-edged sword. It could help accelerate a more seamless payment system without needing to completely blow up the current model and infrastructure...or it could be used to make things exponentially worse. So, between the national momentum for change and the opportunity new technology is bringing, I think we have a fighting chance. It won't happen overnight, but it’s my mission to help eliminate the administrative BS that leads to $300 billion in unnecessary waste and is literally killing patients and providers in the process.
Want more on this topic, including insight-driven research and shared peer-experiences at one of our executive forums?
Be on the lookout for more stories in how payers-providers and related parties are working to ameliorate friction through active collaboration. If you’re interested in speaking with us as part of our ongoing research, please reach out directly at eric@unionhealthcareinsight
Upcoming events
Join our upcoming strategy summit in Chicago on June 2 for a deeper dive on what’s going on in healthcare. Contact Unionevents@unionhealthcareinsight.com for details on how to participate



